Osteoarthritis (OA or arthritis) is the most common joint disease in horses and a survey suggested that 60% of lameness problems are related to OA. Joint pain and loss of mobility due to OA are common causes of poor performance and early retirement in equine athletes. Traumatic injury is considered a common cause of OA and may arise from a single event leading to a joint injury or it may be the result of repetitive, traumatic insults such as the stresses suffered during racing and training.
Traumatic joint disease includes synovitis, capsulitis, articular cartilage damage, ligament damage and OA
- Synovitis – Inflammation of the synovial membrane,
- Capsulitis – inflammation of the fibrous joint capsule,
- Articular cartilage and bone fragmentation or fracture,
- Ligamentous tearing and
- Osteoarthritis – osteoarthritis is the end result of severe injuries and inadequately treated injuries. It is represented by progressive loss of articular cartilage.
Synovitis and capsulitis are the consequence of the trauma suffered by athletic horses during routine training and leads to swelling and pain. If left untreated, the inflammatory mediators released (proteinases, prostaglandins, cytokines and free radicals) in these conditions can contribute to degenerative joint disease, also known as OA. OA is a progressive disease of synovial joints, characterized by degeneration of articular cartilage and clinically associated with pain and lameness. OA is among the most common cause of lameness in horses and is a disease with far reaching economic and welfare implications.
Joint trauma and the arthritis cycle
The environmental effect of trauma on the equine joint initiates and progresses into the arthritis cycle where a negative feedback is experienced and without proper treatment continued degradation will occur.
The pathways of equine traumatic joint disease are on the most part the same as those in osteoarthritis and should traumatic joint disease not be properly treated it will progress along the spectrum to osteoarthritis. Once the arthritis cycle begins, due to its cyclic nature and continual degradation, joint failure will become more frequent leading to additional and more frequent lameness.
A multi-modal approach to these problems is required with a program that prevents and addresses the arthritic cycle and the underlying physical and chemical processes involved.
The arthritis cycle
The arthritic cycle represents the continual degradation and imbalance of chemical and physical processes within the joint. Arthritis can be initiated by a range of external factors, such as joint trauma. Once the arthritis process is initiated there are multiple processes that undergo a deteriorating cycle. Three of these are discussed below and shown in the diagram following.
Cycle 1 – Blood Blockages – An immune response is triggered which causes blood vessel blockages. This leads to poor nutrition to the joint and cartilage degradation. Cartilage degradation then causes further immune response.
Cycle 2 – Joint Fluid Failure – An inflamed joint causes a reduction in the quality and production of joint fluid. With a reduction in the lubrication of the joint, further stress and friction are applied to the joint cartilage. Further cartilage damage results, causing further inflammation.
Cycle 3 – Protein Breakdown – Abnormal joint structure from cartilage failure leads to the production of enzymes that breakdown key joint proteins. These enzymes lead to the breakdown and destruction of cartilage. Further cartilage degradation results in further joint abnormalities and a re-initiation of the cycle.
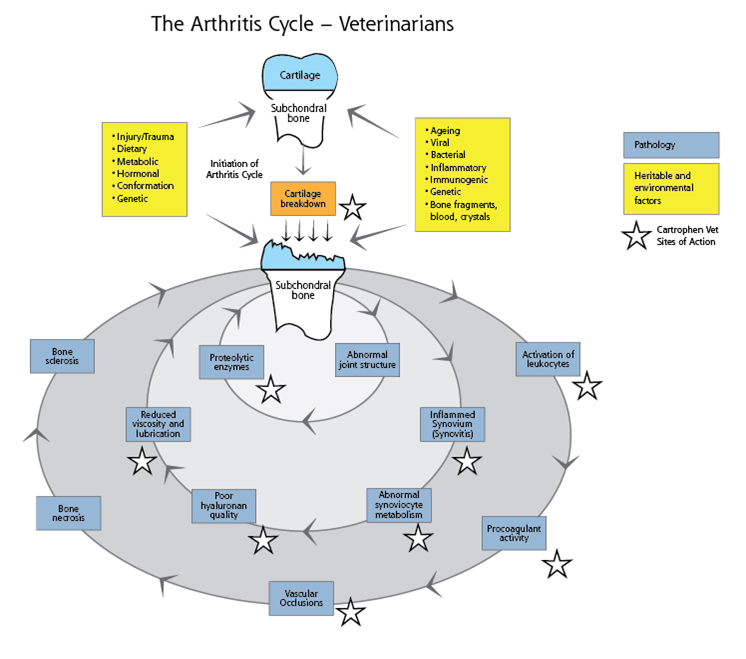
Below is a graphical representation of the arthritis cycle. It shows the healthy joint at the top, with a range of external factors influencing the joint, from hereditary and genetic problems to injuries and trauma. The external factors help initiate the arthritis cycle. Once initiated, there are various pathways of the disease that continually deteriorate without proper treatment and care.
REFERENCES
Click to view referencesCaron JP and Genovese RL (2003) Principles and practices of joint disease treatment. In M.W. Ross and S.J. Dyson (Ed.) Diagnostics and Management of Lameness in the Horse pp 746 -764. Elsevier Science, Philadelphia
McIlwraith CW (1996) In: McIlwraith CW and Trotter GW editors. Joint Disease in the Horse. WB Saunders Company, Philadelphia: 40-70
McIlwraith CW (2011) Traumatic joint injuries and disease. Orthopaedic Research Laboratory, Colorado State University. www.equineortho.colostate.edu/questions/tjd.html Accessed 17 February 2011
Todhunter RJ and Lust G. (1992) In Auer JA, editor. Equine Surgery. WB Saunders Company Ltd, Philadelphia,: 844-866 and Fubini SL et al. (1999) Can J Vet Res; 63:253-260.

